TL;DR:
- Understanding facial anatomy is essential for safe, effective injectables, as improper needle placement can cause serious complications. Recognizing high-risk zones, such as the glabella and nose, helps prevent vascular occlusion and vision loss through precise technique and real-time assessment. Practitioners must continually adapt to individual anatomy variations, maintaining vigilance and swift response to early signs of complications.
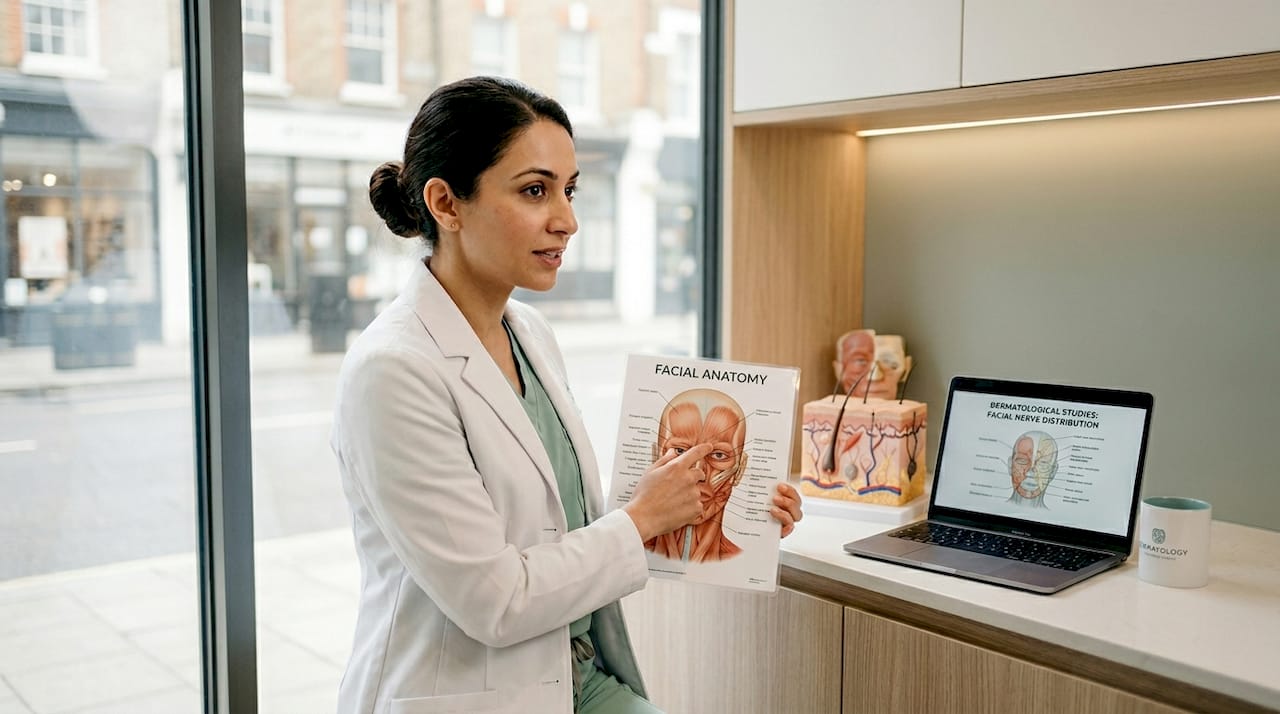
Understanding what lies beneath your skin is not merely academic when it comes to facial injectables. A misplaced needle, a fraction too deep or a millimetre off course, can trigger vascular occlusion, tissue necrosis, or even permanent vision loss. Layered facial anatomy, spanning superficial fat, muscle, deep fat compartments, and proximity to major vasculature, is the single greatest determinant of both aesthetic outcomes and patient safety. This article walks you through the anatomy that matters most: the key facial layers, the danger zones where risks rise sharply, region-by-region risks, and what to do when complications arise.
Table of Contents
- Understanding facial layers: the foundation of safe injectables
- Recognising facial danger zones: where risks rise sharply
- Region-by-region: unique risks, arteries, and safe techniques
- Recognising and reacting to complications: the vascular emergency checklist
- Perspective: what most guides miss about anatomy-led injectable safety
- Explore advanced safe injectables at The Aesthetics Room
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Layer depth is crucial | The specific plane of injection greatly affects safety and the final aesthetic result. |
| High-risk regions exist | Zones like the glabella, nose, and nasolabial folds require added caution due to higher vessel concentration. |
| Fast action saves outcomes | Immediate recognition and prompt intervention are essential for managing vascular complications. |
| Safety needs expertise | Knowledge of individual anatomy and continuous assessment are essential for advanced injectables. |
Understanding facial layers: the foundation of safe injectables
With the high stakes in mind, it is essential to begin by breaking down the key structural layers of the face. These layers form the map every skilled injector works from, and understanding them helps you ask better questions and make more informed decisions about your treatment.
The face is built in five primary layers, each with distinct properties and clinical implications:
- Skin (dermis and epidermis): The outermost layer. Superficial injections here, such as skin boosters and some fine-line treatments, carry the lowest risk of vascular events.
- Superficial fat compartments (subcutaneous fat): These lie just beneath the skin and are further divided into discrete compartments that change volume with age. Superficial fillers placed here can spread unpredictably if the compartment boundaries are not respected.
- SMAS and muscle layer: The superficial musculoaponeurotic system (SMAS) and the underlying facial muscles are where botulinum toxin (Botox) works to relax dynamic wrinkles. Penetrating too deep when intending a superficial injection risks hitting structures that should be avoided.
- Deep fat compartments: Located beneath the SMAS, these compartments sit in close proximity to major vessels and nerves. Injections here carry significantly higher risk and require precise anatomical knowledge.
- Periosteum and bone: The deepest layer, where some structural filler placements are deliberately made, particularly over the cheekbone or chin. This plane can actually be safer for volume augmentation in certain regions because the vasculature is less dense immediately above the bone.
Understanding facial anatomy and cosmetic safety is the foundation on which every injectable decision is built. As modern injectable safety research confirms, depth is a primary determinant of both aesthetic spread and complication risk. A product placed in the wrong layer can migrate, cause vascular compression, or, in the worst case, be inadvertently injected intravascularly.
| Facial layer | Typical products used | Primary risks |
|---|---|---|
| Skin / intradermal | Skin boosters, fine-line toxin | Bruising, superficial nodules |
| Superficial fat | Light hyaluronic acid fillers | Tyndall effect, migration |
| SMAS / muscle | Botulinum toxin | Ptosis, asymmetry if off-target |
| Deep fat | Structural fillers (e.g., calcium hydroxyapatite) | Vascular occlusion, nerve compression |
| Periosteum / bone | Volumising fillers, structural support | Periosteal pain, rare vascular events |
The role of fillers in facial layers is nuanced. Not every product suits every layer, and the best results come from matching the filler’s rheology (its thickness and flow characteristics) to the specific compartment being treated.
Pro Tip: Applied, layer-based mapping for injectables is far more clinically useful than reading surgical anatomy textbooks. Surgical texts describe anatomy in terms of dissection planes, whereas injectable practice demands a three-dimensional, live-tissue appreciation of how layers shift with movement, age, and individual variation.
Recognising facial danger zones: where risks rise sharply
Beyond the layers, being aware of precise anatomical danger zones is critical for anyone considering advanced injectables. These are regions where major arteries and veins run in close proximity to the surface, or where direct connections to the ophthalmic circulation make a vascular event immediately sight-threatening.
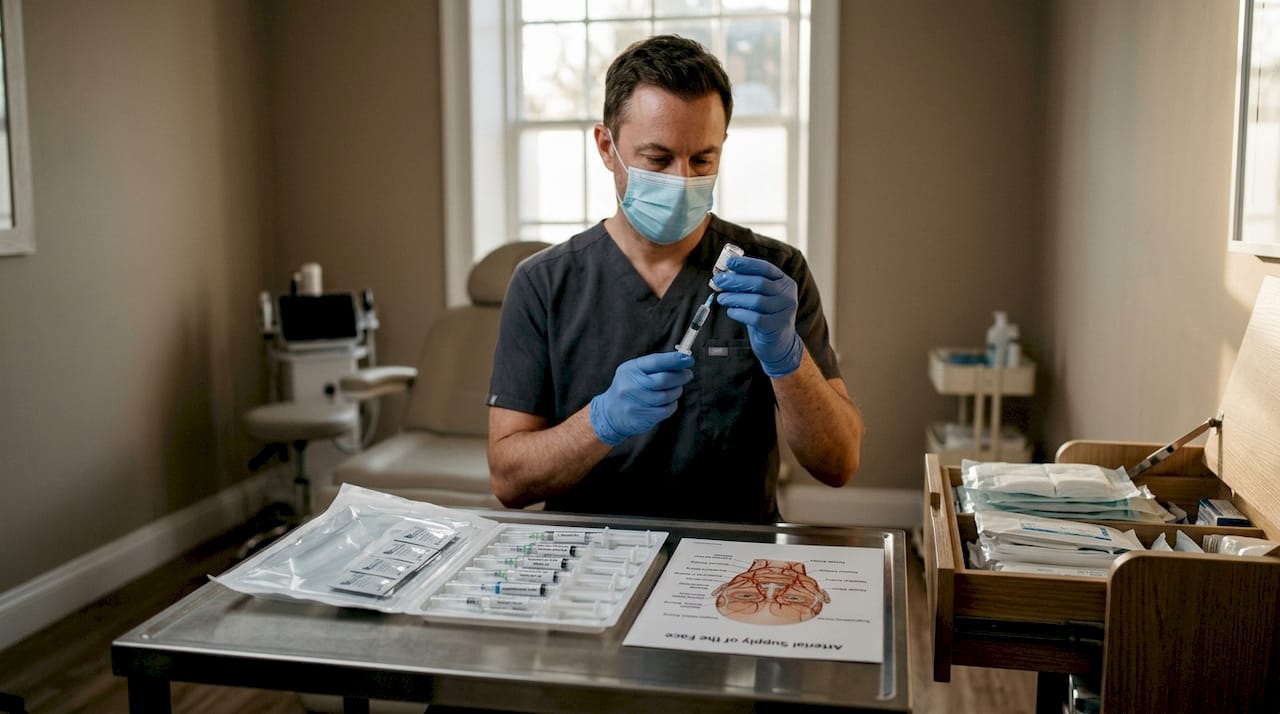
Research published in Plastic and Reconstructive Surgery confirms that danger zones are region-specific and depth-dependent, and that mapping technique to vessel location meaningfully reduces injury risk. A large analysis of vascular occlusion cases further shows that high-risk anatomical zones including the glabella, nose, and nasolabial folds account for a disproportionate share of occlusive events.
The six major danger zones every patient should know about are:
- Glabella (between the brows): Highest risk zone. The supratrochlear and supraorbital arteries branch here. Retrograde embolism can reach the ophthalmic artery within seconds.
- Nasal region: The dorsal nasal artery and lateral nasal artery connect directly to the ophthalmic circulation. Filler here can cause skin necrosis of the nose or catastrophic vision loss.
- Nasolabial folds: The angular artery runs along this fold and communicates with orbital vessels. Overfilling or incorrect depth creates significant occlusion risk.
- Temples: The superficial temporal artery and its branches lie close to the skin surface here. Incorrect placement can cause scalp or forehead necrosis.
- Tear trough: Proximity to the infraorbital vessels and the orbit itself makes this a zone that demands conservative volumes and precise depth.
- Lips: The superior and inferior labial arteries run within the orbicularis muscle. Intravascular injection here can cause significant lip necrosis.
| High-risk zone | Primary danger | Consequence | Mitigation tactic |
|---|---|---|---|
| Glabella | Supratrochlear / supraorbital artery | Vision loss, forehead necrosis | Aspirate, use cannula, low volumes |
| Nose | Dorsal / lateral nasal artery | Nasal tip necrosis, blindness | Micro-bolus technique, periosteal placement |
| Nasolabial fold | Angular artery | Skin necrosis, orbital involvement | Cannula preferred, avoid medial placement |
| Temple | Superficial temporal artery | Scalp / forehead necrosis | Deep periosteal or superficial subdermal only |
| Tear trough | Infraorbital vessels | Bruising, vision risk | Very small volumes, blunt cannula |
| Lips | Labial arteries | Lip and perioral necrosis | Aspirate, linear threading technique |
Risk is not uniform across these zones. It depends on the direct vascular connections each area shares with the ophthalmic circulation. The transformative areas for fillers that create the most dramatic aesthetic improvement are, in many cases, the same zones that carry the highest vascular risk. That is not a reason to avoid them; it is a reason to choose your practitioner very carefully.
Top tips for patients considering treatment in these zones:
- Always ask whether your practitioner carries hyaluronidase (the emergency reversal enzyme for hyaluronic acid fillers) on-site.
- Ask about the use of blunt cannulas versus sharp needles, especially near the nose and nasolabial folds.
- Confirm that your provider conducts a full facial vascular mapping assessment before any high-risk treatment.
- Request small initial volumes in danger zones and review results before adding more product.
Region-by-region: unique risks, arteries, and safe techniques
Understanding general danger zones is only the start. Different facial regions present their own distinct anatomical challenges, and a truly safe approach requires working through the face systematically.
-
Forehead: The supraorbital and supratrochlear arteries exit the orbit at the brow and run superiorly. Toxin placed here to soften horizontal lines must avoid the levator muscle of the upper lid. Fillers for brow lifting carry real risk if placed too deeply near these exit points.
-
Glabella: The most cited danger zone in the literature. The supratrochlear artery is the primary concern. Even a tiny volume of filler injected intravascularly here can cause bilateral blindness because of direct anatomical connections to the central retinal artery. Technique here demands extreme precision, very low pressure, and ideally a cannula approach.
-
Temples: Hollowing here is a common sign of facial ageing, and volumising the temples creates significant rejuvenation. However, the superficial temporal artery runs just beneath the skin in this region. Injecting at the periosteal level is generally safer, though the middle temporal vein also lies in a potential injection corridor and can cause significant haematoma.
-
Cheeks: The midface is a more forgiving region anatomically, but the infraorbital foramen sits approximately 1 cm below the orbital rim in the midpupillary line. The infraorbital nerve and vessels exit here, making this an important landmark to avoid with deep injections.
-
Tear trough: This is one of the most technically demanding areas. The orbicularis muscle is thin here, and incorrect plane placement leads to chronic oedema, the Tyndall effect (a bluish discolouration from superficially placed filler), or vascular events. Only highly dilute, low-viscosity hyaluronic acid fillers should be used, in conservative volumes.
-
Lips: The labial arteries run centrally within the body of the lip, inside the orbicularis oris muscle. Safe technique involves either supra-muscular or sub-muscular placement, never directly within the muscle belly at the midline.
-
Chin and jawline: Relatively safer zones, though the mental nerve exits the mental foramen on each side of the chin, making deep midline injections above the foramen a point of care. The facial artery courses along the jawline and must be respected during lower face volumisation.
As facial assessment research consistently emphasises, slow, careful, and methodical technique with constant attention to local anatomy minimises complications across every region.
“Safety in facial injectables is not achieved by memorising a diagram. It is achieved by the practitioner maintaining continuous, real-time awareness of how deep the needle is, what resistance they feel, and what the tissue response looks like at every moment of injection.”
Pro Tip: So-called safe zones can change between individuals and even between sessions for the same individual. Weight loss, previous filler, scarring, and natural anatomical variance all shift vessel positions. Your practitioner’s ability to adapt their approach in real time is what separates good outcomes from serious complications. For those seeking guidance on achieving natural results, these subtle filler tips offer excellent practical context.
Recognising and reacting to complications: the vascular emergency checklist
Knowing the anatomy is only part of safe injectable practice. Rapid recognition and action in emergencies completes the safety picture, and every patient should understand the warning signs.
Vascular occlusion, where an artery or vein becomes blocked by filler material, is the most serious acute complication from dermal fillers. It can occur in seconds. The early signs are:
- Immediate blanching (whitening) of the skin: This is the most reliable early sign. If the skin turns white or greyish at the injection site or in a distribution beyond it, vascular compromise is occurring.
- Pain out of proportion to the procedure: Sharp, burning, or intense pain during injection should prompt immediate cessation.
- Visual disturbance: Any changes in vision, including blurring, darkening, or visual field loss, represent an ophthalmic emergency.
- Slow capillary refill: Pressing on the affected skin and observing delayed return of colour (more than 2 seconds) indicates compromised perfusion.
- Skin mottling or dusky discolouration: This appears as the occlusion progresses and tissue oxygen levels fall.
The intervention window matters enormously. Research confirms that treatment within the first 4 to 6 hours is associated with significantly improved prognosis for cutaneous vascular occlusion cases. Hyaluronidase, injected into and around the affected area, dissolves hyaluronic acid filler and can restore circulation if administered promptly.
The ophthalmic risk is even more time-critical. Retinal ischaemia can become irreversible within 12 to 15 minutes of onset. This is why practitioner readiness, including immediate access to hyaluronidase and a clear emergency protocol, is non-negotiable.
Patient awareness is equally important. Knowing how to prepare for injectable treatments safely and understanding these warning signs means you can communicate clearly and immediately if something feels wrong during or after your procedure.
Perspective: what most guides miss about anatomy-led injectable safety
All the evidence above points to one crucial realisation: facial anatomy for injectables is not static and not one-size-fits-all. Most guides present danger zone diagrams as though they are universal truths. They are not. They are useful approximations built on cadaver studies, and real people differ in ways those studies cannot fully capture.
We have seen a genuine and productive debate emerge in the literature between two models of risk. One model treats danger zones primarily as depth-dependent vessel risks, where knowing the right layer is sufficient. The other uses a broader, classification-based risk model that accounts for occlusion management, vessel redundancy, and individual variation rather than just location labels. Both contribute meaningfully, but neither alone is adequate.
The uncomfortable truth is that even experienced practitioners can encounter unexpected vessel positions. What matters most is not a fixed injection map but the practitioner’s capacity for ongoing learning, honest self-assessment, and genuine humility when anatomy surprises them. Complacency is the real risk factor.
Our perspective at The Aesthetics Room is clear: the best practitioners are those who never stop studying ongoing anatomical learning and who treat every face as a unique anatomy to be assessed, not a template to be filled.
Pro Tip: Before any advanced injectable treatment, ask your provider to describe their anatomical assessment plan for your specific face. If they cannot explain which vessels they are avoiding, how deep they intend to inject, and what their emergency protocol is, that is important information. Confidence in your provider’s knowledge is as important as confidence in the product.
Explore advanced safe injectables at The Aesthetics Room
If you’re ready to put evidence and expert perspective into safe, beautiful practice, the right guidance and provider make all the difference.
At The Aesthetics Room, our clinicians bring genuine anatomical expertise to every injectable consultation. We do not work from templates. We assess your individual facial structure, discuss your goals, and build a treatment plan that prioritises your safety and your results in equal measure. Whether you are considering expert dermal fillers to restore volume and structure, exploring why choose fillers in London for the first time, or looking into specialist Botox treatments for natural-looking rejuvenation, our team is here to guide you with knowledge, care, and clinical precision. Book your consultation today and experience the difference that anatomy-led practice makes.
Frequently asked questions
What are the main facial danger zones for injectable treatments?
The highest risk regions are the glabella, nose, and nasolabial folds, which carry the greatest risk for vascular complications due to their direct connections to the ophthalmic circulation, as confirmed by vascular occlusion risk data.
Why is the depth of injection so important for safety?
Injection depth determines which vessels or structures are at risk and directly influences both the effectiveness and safety of the procedure, with layered facial anatomy being the primary map for safe injectable practice.
How can vascular complications from injectables be recognised early?
Early warning signs include skin blanching, pain, and visual changes, with the initial 4 to 6 hour window being critical for hyaluronidase intervention and improved outcomes.
Can vision loss from filler complications be reversed?
Vision loss can become permanent within minutes, so immediate recognition and intervention are essential, as retinal ischaemia following filler embolisation can become irreversible rapidly, with full recovery being rare after prolonged non-perfusion.
Does each face have the same safe zones for injectables?
No. Individual variation in vessel location, depth, and tissue structure means that safe zones differ between patients and can shift over time due to factors such as previous filler placement, weight changes, and natural anatomy.
Recommended
- Facial anatomy: the key to safer cosmetic results – The Aesthetics Room
- Injectables in Aesthetics: Subtle Enhancement Explained – The Aesthetics Room
- Why choose injectables? Benefits, safety and results – The Aesthetics Room
- Injectable contouring: achieve refined, natural results safely – The Aesthetics Room